Trochanteric Bursitis
Summary
Trochanteric bursitis occurs when the tissue (bursa) over the prominent bone on the outside of the hip (greater trochanter) becomes inflamed from either an acute injury or repetitive irritation. Trochanteric bursitis is more common in females than males. It is also more common in middle aged and elderly persons. Repetitive activities causing injury to the bursa such as running, stair climbing, bicycling, prolong standing, and injury to the hip can result in the development of trochanteric bursitis.
Treatment for trochanteric bursitis is largely non-operative. This includes the use of non-steroidal anti-inflammatory medications, activity modification, corticosteroid and local anesthetic (freezing medication) injections, and physical therapy –including stretching. Surgical treatment, which includes removal of the bursa, is rarely needed and is reserved for severe cases that do not respond to non-surgical management.
Clinical Presentation
A bursa is a thin fluid-filled sac that overlies bony protrusions to provide protection, as well as reduce friction as muscles and tendons slide over the bone. The trochanteric bursa lies over the greater trochanter of the femur, creating a layer of protection between the iliotibial (IT) band and greater trochanter as the IT band moves over this area during hip flexion and extension (figure 1). Inflammation of the trochanteric bursa can occur if the IT band becomes tight, increasing friction over the surface of the bursa. This leads to lateral hip pain located over the greater trochanteric region.
Figure 1: Image showing the location of the greater trochanteric bursa
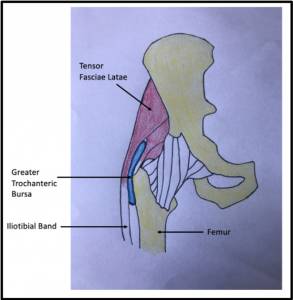
Trochanteric bursitis is more common in middle-aged and elderly females, but can also occur in males. It is commonly associated with repetitive activities such as running, stair climbing, bicycling, prolonged standing and acute injuries or trauma to the hip. However, it can also be precipitated by a direct blow to the greater trochanter on the outside of the hip. The most common symptom patients complain of is hip pain localized to the lateral aspect, or outside, of the hip and specifically over the greater trochanter. The pain can be sharp or dull and can extend down the outside of the thigh. The pain is usually worse at night and when lying on the affected side, which places pressure on the bursa. Lying on the unaffected side can also cause pain because this increases the stretch on the IT band lying over the hip with trochanteric bursitis, which can worsen inflammation. Activities such as running and walking can also worsen symptoms.
Physical Exam
While there are not many specific exam findings for trochanteric bursitis, the exam is important in order to rule out other causes of hip pain. The most common finding of trochanteric bursitis is tenderness elicited when applying pressure over the greater trochanter. Other signs of inflammation may be present such as swelling of the bursa, but these are usually difficult to see as the bursa lies below skin and muscles.
Imaging
X-ray is usually not helpful in the diagnosis of trochanteric bursitis as the bursa is a soft tissue and x-rays are most useful for visualizing bone. X-rays are ordered for this condition to rule out other diagnoses, although in some patients a small spike of bone or a rough area of bone may be observed associated with the outside (lateral aspect) of the greater trochanter.
An MRI is useful for demonstrating inflammation in the bursa that can be suggestive of trochanteric bursitis. However, an MRI is not routinely used due to the expense, unless there is a specific reason, such as severe bursitis that is unresolved with treatment.
An ultrasound is another option for visualizing a swollen trochanteric bursa and if may also facilitate an accurate injection into the bursa.
Non-operative Treatment
The first line of treatment for trochanteric bursitis is non-operative management. This involves activity modification to avoid activities that worsen symptoms. The use of NSAIDs and steroid injections into the bursa can help to relieve pain and reduce inflammation. Physical therapy and at-home stretching exercises that focus on restoring flexibility to the IT band can help reduce the friction placed on the trochanteric bursa, thus reducing inflammation and pain.
Operative Treatment
Surgery is rarely needed for trochanteric bursitis. However, if symptoms persist despite utilization of all non-operative measures, surgical removal of the bursa can be performed along with smoothing out any rough areas of the adjacent bone. This surgery is usually done by opening up the skin, although in some patients it may be possible to perform the surgery arthroscopically. Both open and arthroscopic bursa removal have short recovery times.
