Intertrochanteric Hip Fracture
Summary
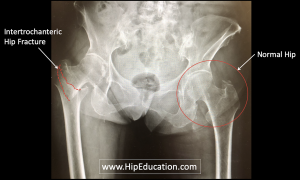
Intertrochanteric hip fractures occur between the greater and lesser trochanter of the femur (figure 1). The greater trochanter protrudes from the outside (lateral aspect) of the femur, while the lesser trochanter protrudes from the inside (medial aspect) of the femur. Both serve as attachment points for muscles that move the hip joint. There is abundant blood supply in the intertrochanteric region because this region is outside of the hip joint capsule (extracapsular). Therefore, there is a decreased risk of avascular necrosis and failure to heal (non-union) compared with femoral neck fractures.
Intertrochanteric hip fractures can be either stable or unstable. Stability refers to whether or not the fracture is in multiple pieces (comminuted) and whether or not the fracture is in danger of displacement when a load is applied to the affected leg.
Intertrochanteric hip fractures are caused by low-impact falls in the elderly, or less commonly by high impact falls in younger individuals. Consequences of this type of fracture include a risk of permanent disability (morbidity) and possibly death (mortality) if left untreated. Treatment options for intertrochanteric hip fractures are largely surgical and include a dynamic hip screw or trochanteric femoral nail.
Figure 1: X-ray of an intertrochanteric hip fracture.
Clinical Presentation
Intertrochanteric hip fractures occur more often in females than males. Elderly individuals, especially those with osteoporosis and a history of falls are also more likely to suffer from this type of fracture. A person presenting with an intertrochanteric hip fracture will usually be elderly and give a history of a recent low-impact fall from ground level. They will find it difficult or impossible to place weight on the affected leg. If they are able to walk, they will present with a marked limp favoring the unaffected side.
Physical Exam
On examination, there will be significant pain in the hip region and swelling over the area of the greater trochanter when compared to the unaffected hip. There may also be bruising over the area that was impacted when the initial fall occurred. The affected leg will often appear shortened and rotated outward (externally rotated). In rare cases where the nerves in the area have been impacted as a result of the fracture, there may be numbness and tingling or a loss of some sensation in various areas around the hip and thigh.
Imaging
X-rays are the most valuable form of imaging when diagnosing a hip fracture. X-rays will provide a clear image of the bones and will reveal the location of the fracture line. They will also reveal whether or not the fracture is in multiple pieces. X-rays can be used to evaluate the stability of the fracture, and therefore which surgery is appropriate for treatment.
A CT or MRI scan may be ordered if the x-rays do not show a fracture, but suspicion of a fracture is still high given the nature of the injury and findings on physical exam. CT and MRI can reveal stress or hairline fractures, which are incomplete fractures where there is no clear fracture line seen on plain x-ray.
Non-operative Treatment
In general, surgery to stabilize the fracture is the recommended treatment option to ensure the best possible recovery after an intertrochanteric hip fracture. However, very rarely in higher risk patients and/or patients who were not able to walk prior to the injury (non-ambulatory), surgery may not be an option. Patients will be in bed and non-mobile prior to surgery.
Operative Treatment
There are 2 surgical procedures that are typically used in the treatment of intertrochanteric hip fractures: a dynamic hip screw or a trochanteric femoral nail. The type of procedure performed depends on the nature of the fracture as well as the individual characteristics of the patient. These procedures require that the fractured bones be appropriately realigned prior to inserting the surgical hardware. This is achieved by placing the patient in traction on a special operating table (fracture table) and checking the fracture position with a special portable x-ray machine (fluoroscopy).
Dynamic Hip Screw
A dynamic hip screw is a good procedure to treat stable intertrochanteric hip fractures. A strong screw is placed across the fracture site into the femoral head –the ”ball” part of the hip joint. This is done using fluoroscopy. A strong metal plate is placed along the outside of the thigh bone and secured with screws. The hip screw is then able to slide along the groove at the top of the plate that when loaded creates a continuous dynamic force across the fracture site. This force promotes faster healing of the fracture. This device is sometimes referred to as a “sliding hip screw”.
Trochanteric Femoral Nail
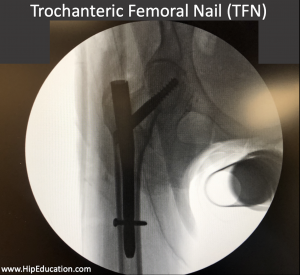
Trochanteric femoral nail placement is suitable for either stable or unstable fractures (figure 2). It involves placing a short or long nail through the center of the femur and then positioning a “hip screw” across the fracture site into the femoral head. In stable fractures, the hip screw may be allowed to slide to compress the fracture site. In unstable fractures, the screw may be locked to prevent the fracture from collapsing.
Figure 2: X-ray of a trochanteric femoral nail
A third procedure, total hip replacement, is used rarely -specifically in cases of severe bone fragmentation (comminution). It can also be used in persons who have preexisting osteoarthritis or fractures that have failed to heal using the two surgical procedures discussed above.
Patient References Websites
- https://orthoinfo.aaos.org/en/diseases–conditions/hip-fractures
- https://stanfordhealthcare.org/medical-conditions/bones-joints-and-muscles/hip-fracture/types.html