Total Hip Replacement (Total Hip Arthroplasty)
Indications
A total hip replacement helps can alleviate the pain associated with severe hip arthritis and restore function to the hip joint. It is recommended for treatment of moderate to severe hip arthritis; hip fractures that have failed to heal (nonunion) despite undergoing internal fixation; and in cases of advanced bone death (avascular necrosis) of the femoral head.
Procedure
Overview
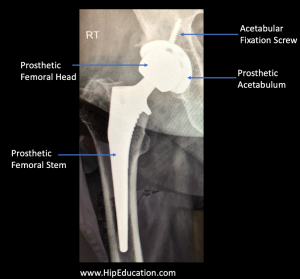
The artificial hip joint consists of a prosthetic acetabulum (socket); a prosthetic femoral head (ball) that glides over the acetabulum; and a prosthetic stem that inserts into the femoral head on one side and the existing healthy femoral shaft (thigh bone) on the other (figure1).
Figure 1: X-ray of a total hip replacement (arthroplasty)
Femoral component
The prosthetic femoral shaft component, or stem, is inserted into the shaft of the existing femur. The thigh bone is prepared to receive the femoral prosthesis by creating a progressively larger hollowed out area using increasingly larger surgical tools called femoral broaches. The actual femoral prosthesis is secured in place either via a press-fit, or by using bone cement. A “press-fit” femoral prosthesis relies on bone ingrowth for long-term stability –bone from the patient grows around small beads on the surface of the femoral prosthesis. A “cemented” femoral prosthesis is stabilized by injecting bone cement into the hollowed out femoral canal and them placing the femoral component into the putty-like cement before it hardens. When the bone cement dries it creates a strong secure interface between the patients bone and the metal femoral component.
Femoral head
A prosthetic “ball” is placed on top of the stem to replicate the head of the femur. This ball is very smooth and usually made of a special metal or ceramic. The femoral head moves within the acetabular prosthesis and thereby serves as one side of the mobile interface between the femoral and acetabular prosthetic components.
Acetabular component (Hip socket)
The artificial acetabulum usually has two components -a metal cage, and a cup-like component that is snapped into the metal cage and serves as the interface with the smooth femoral head. The metal cage is attached to the disease-free pelvic bone after preparing the arthritis hip socket to accept the acetabular prosthesis. The acetabular component is secured into the pelvis either using press-fit (bone ingrowth possible augmented with screws), or bone cement.
The artificial components glide smoothly against each other during hip movement, mimicking the function of a healthy hip joint. Hip joint replacements differ in the material the prosthetic parts are made of, how the prosthesis is fixed to the body, and the surgical approach used. Each of these differences is outline below.
Prosthetic Components
The femoral component of the prosthesis consists of a metal or ceramic head, and a metal stem. The stem is implanted inside the femur after the femoral head and neck are removed, and additional bone is removed to make space for the stem. The artificial head is attached to the free end of the stem. The acetabular (socket) component is placed within the acetabulum after cartilage and diseased bone have been removed. It often consists of a metal cage with the bearing surface inside the cage being made of high molecular weight polyethylene (plastic), ceramic, or metal.
The final component of the artificial hip is the bearing surface or articulating surface. A bearing surface is the surface of the femoral head prosthesis and the surface of the prosthetic acetabulum that come into contact with each other. The type of surface to be used depends on a person’s age, level of activity, and the preference of the surgeon. The standard bearing surface has been metal on polyethylene. Metal-on-metal (a metal acetabular surface and a metal femoral head) is no longer used because it was found to release metal into the blood stream, which may have toxic effects. Here is a brief overview of the common bearing surfaces used today:
- Metal-on-polyethylene – Metal femoral head and polyethylene acetabulum. This is currently the most common bearing surfaced used in total hip replacement. Metal-on-polyethylene is suitable for individuals above the age of 65 and those who lead a more sedentary lifestyle.
- Ceramic-on-polyethylene – The femoral component is ceramic and the acetabular component is made of polyethylene. One advantage of the ceramic head is that it produces less friction when sliding over the acetabular surface as compared to metal.
- Ceramic-on-ceramic – Ceramic acetabular component and ceramic femoral head. This type of replacement is most commonly used in active individuals under the age of 60. Ceramic-on-ceramic can also be used between age 60 and 65 depending on the individual’s level of activity. The ceramic components create less friction than metal when sliding against each other, and generally last longer than other types of hip replacements. One disadvantage of this type of replacement is that it may produce a “squeaking” noise with movement.
Fixation of the Hip Replacement: Cemented vs. Uncemented
The two types of fixation methods used in hip replacement surgeries that help adhere the prosthesis to the existing bone are cemented and uncemented. Cemented hip replacements use a bone cement that adheres the prothesis to the bone, while uncemented hip replacements have a textured surface that promotes bone ingrowth and adherence of the hardware to the bone overtime. A hip replacement can also be fixed to bone by a combination of these two methods.
The cemented hip replacement is preferred for older individuals. Advantages of a cemented hip replacement include placement of the prosthesis without risk of movement or misalignment after it has been placed; rapid stability of the prosthesis as the bone cement hardens during surgery and can bear full weight immediately (unlike an uncemented prosthesis which requires weeks or months for adequate bone ingrowth to stabilize the prosthesis); and the ability to insert an antibiotic into the cement to prevent infection. Disadvantages include risk of cement breakdown over time that can cause a reaction in the lining of the hip joint. The bodies resulting inflammatory response can eventually lead to breakdown bone (osteolysis) resulting in prosthetic loosening.
Uncemented hip replacements are more commonly used in younger individuals who have healthier bone. The advantages of this type of fixation include eliminating the risk of cement breakdown and possible improved long-term adhesion of the prothesis to the bone. The main disadvantage is that it takes a long time for new bone to form, so the prosthesis is not fixed in place directly after surgery, meaning that patients must limit their weight bearing for an extended period of time after the surgery.
Surgical approaches to the Hip Replacement
Total hip replacements can be performed using a few different techniques to create a window to “approach” the hip joint. Each surgical approach has their own risks and benefits. The technique that is used depends on the preference and experience of the surgeon, as well as what will best suit the patient undergoing surgery. In general, different techniques require disruption of different muscles, tendons, and ligaments in the body. Although these structures heal with time, they may never fully return to their original condition. The 3 main approaches to a hip replacement are as follows:
- Posterior approach – The posterior approach is useful for more complex cases, as well as for revision total hip replacements. It allows for good exposure of the hip joint. It does not have an increased rate of prosthetic failure like the anterior approach. However, it may have a higher rate of hip dislocation compared to the other approaches.
- Lateral approach – The Lateral approach requires the patient to be lying on their side and allows for good visualization of the socket (acetabulum). However, complications including abnormalities with walking after recovery from surgery and increased risk of abnormal bone growth in non-bony tissue (heterotopic ossification) make this approach less commonly utilized than the posterior approach.
- Anterior approach – In this technique, the patient is lying on their back during surgery. This approach is advantageous because it does not require any major tendons to be cut during the surgical approach. Therefore, it generally allows an individual to stop using a cane, walker, or other assistive device earlier than is typical for the other approaches. However, the anterior approach can be problematic because the surgical exposure of the hip joint is more limited. It is therefore a much more challenging procedure from a technical point of view. As a result, it is associated with a slightly higher rate of failure of the prosthetic component responsible for replacing the femur due to limitations during surgery. As such, it is the least common approach.
Recovery
An important part of recovery from total hip replacement is early mobilization using an assistive device such as a cane or walker. Individuals who undergo total hip replacement are encouraged to begin placing weight on the hip almost immediately after surgery. During the recovery period, increasing increments of body weight will be placed on the hip until walking without an assistive device is achieved. Total hip replacement surgery is associated with an increased risk of developing a blood clot (deep vein thrombosis). To prevent this, blood thinners such as aspirin and the use of compression stockings to help return blood flow to the heart are highly recommended.
Physical therapy and in-home exercises are also a key component of recovery. Specific exercises designed to promote strength and stability of the hip, when performed regularly after a total hip replacement, will help achieve the maximum possible activity level after surgery. The physical therapist will also provide guidelines for preventing hip dislocation during and after the recovery period, as artificial hips are more prone to dislocation.
Complications
Potential complications of a total hip replacement include:
- Surgical site infection
- Deep vein thrombosis and pulmonary embolism
- Failure of the prosthesis
- Leg-length discrepancy, or one leg being shorter than the other
- Loosening of the prosthesis
- Hip dislocation
- Heterotopic ossification, or bone formation in a place where it is not supposed to form